Enhanced Healing Agents
Enhanced Healing Agents
Enhanced Healing using Modern Science
Wound healing and the science behind it are an integral part of plastic surgery. The cascade of wound healing is integral to every plastic surgery operation that is done. Whether it is simple suturing of a wound or incision or during a complex surgery, no medical specialty is faced with more diverse wound healing challenges. Plastic surgery offers a wide spectrum of wound healing methods from tissue flaps, skin and fat grafting to topical therapies. Several exciting new technologies use products harvested from one’s own blood and body tissues such as platelet-rich plasma (PRP) and fat (stem cells). Others use biologic scaffolds derived from human or animal sources such as Alloderm or Matristem. Depending upon the wound healing problem or tissue deficiency, the concept is that these agents encourage accelerated wound healing, tissue ingrowth and even tissue replacement in some cases. By aiding the body’s natural healing processes, new natural tissue develops that may result in less scarring and faster healing than would normally occur.
Platelet-Rich Plasma
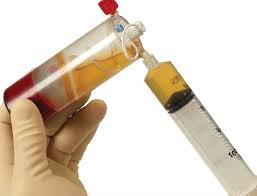
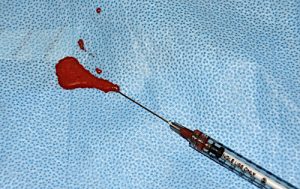
 PRP (platelet-rich plasma) is a natural concentrate of one’s own blood that contains platelets and other growth factors. By drawing a small amount of blood, it is centrifuged and a concentration or plug of platelets is obtained. This can be injected into wounds, mixed with other wound healing agents, or sprayed onto the surface of the wound. Because it is natural and contains potent healing agents, it has become popular for many wound and surgical procedures. It is often used today as an adjunct to such aesthetic procedures as facelifts, facial laser resurfacing, fat grafting and hair revitalization.
PRP (platelet-rich plasma) is a natural concentrate of one’s own blood that contains platelets and other growth factors. By drawing a small amount of blood, it is centrifuged and a concentration or plug of platelets is obtained. This can be injected into wounds, mixed with other wound healing agents, or sprayed onto the surface of the wound. Because it is natural and contains potent healing agents, it has become popular for many wound and surgical procedures. It is often used today as an adjunct to such aesthetic procedures as facelifts, facial laser resurfacing, fat grafting and hair revitalization.
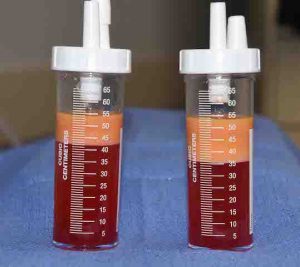
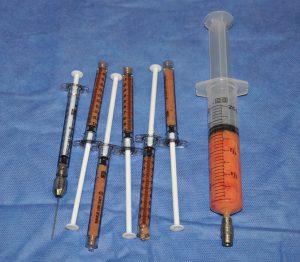
 While fat can be removed by liposuction, it has historically been discarded. Now recognized as containing stem cells and other growth factors, it is being ‘recycled’ in patients for the aesthetic treatment of injectable volume additions to the face, breasts, buttocks and specific soft tissue defects anywhere on the body. Being a natural product and one that most everyone has a little too much of, it is harvested by liposuction techniques and concentrated to include mainly the cellular material. In this cellular milieu is an assortment of stem cells, while whether and how they work is not yet fully understood, their value to an injected fat concentrate is believed to improve its survival. Finer concentrates of fat, known as nanofat, can be used for injection into smaller tissue sites where more traditional fat concentrates are too thick. Such fat graft concentrates are commonly combined with PRP (platelet-rich plasma) to have synergistic effect of improved healing along with better fat survival.
While fat can be removed by liposuction, it has historically been discarded. Now recognized as containing stem cells and other growth factors, it is being ‘recycled’ in patients for the aesthetic treatment of injectable volume additions to the face, breasts, buttocks and specific soft tissue defects anywhere on the body. Being a natural product and one that most everyone has a little too much of, it is harvested by liposuction techniques and concentrated to include mainly the cellular material. In this cellular milieu is an assortment of stem cells, while whether and how they work is not yet fully understood, their value to an injected fat concentrate is believed to improve its survival. Finer concentrates of fat, known as nanofat, can be used for injection into smaller tissue sites where more traditional fat concentrates are too thick. Such fat graft concentrates are commonly combined with PRP (platelet-rich plasma) to have synergistic effect of improved healing along with better fat survival.
While PRP can be used alone, a variety of procedures have been developed that combine it with different types of injectable fillers. Marketed brand names such as Selphyl and the Vampire Facelift create either a platelet-rich fibrin matrix or are used in conjunction with other well-known fillers such as Juvederm and Restylane. The benefits of PRP in these facial rejuvenation techniques, though appealing, have not been fully substantiated in widespread clinical use, and the cosmetic surgery community continues to evaluate the efficacy of this autologous therapy.
ACELL

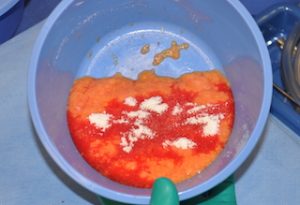 MatriStem (Acell) is a non-synthetic implant that is completely resorbable and acellular. It is a unique implant because it induces healing by triggering extensive new blood vessel formation and recruiting specific cell types to heal the wound site. These cells have the potential to become tissue that is natural to the specific tissue site rather than undifferentiated scar tissue. During the healing process, the implant material is completely resorbed, leaving behind natural tissue replacement and not just a scar or an unnatural residual implant. Less scarring means more natural tissue replacement, which can improve the appearance of the scar and lead to improved mobility and function of the specific body part or surgical site. MatriStem is currently available in both sheet and micronized particle form (powder). The availability of these two forms allows the material to be applied to any surgical site. Its use in powder form is applicable to any surgical site. Matristem can also be mixed in with fat grafting for a unique combination of enhanced healing agents.
MatriStem (Acell) is a non-synthetic implant that is completely resorbable and acellular. It is a unique implant because it induces healing by triggering extensive new blood vessel formation and recruiting specific cell types to heal the wound site. These cells have the potential to become tissue that is natural to the specific tissue site rather than undifferentiated scar tissue. During the healing process, the implant material is completely resorbed, leaving behind natural tissue replacement and not just a scar or an unnatural residual implant. Less scarring means more natural tissue replacement, which can improve the appearance of the scar and lead to improved mobility and function of the specific body part or surgical site. MatriStem is currently available in both sheet and micronized particle form (powder). The availability of these two forms allows the material to be applied to any surgical site. Its use in powder form is applicable to any surgical site. Matristem can also be mixed in with fat grafting for a unique combination of enhanced healing agents.
BIOBURST REJUV
 Another useful enhanced wound healing agent is BioBurst Rejuv. This is an umbilical cord blood (UCB) derived cellular allograft which has been shown to initiate regeneration of soft tissue. When applied into surgical site it uses the body’s own natural healing process to signal molecules to initiate a regenerative response. Essentially signaling molecules recruit the body’s stem cells to the site of injury and cause them to proliferate. These stem cells promote a regenerative response with the formation of matrix proteins and blood vessels. While much attention has been given to adipose derived stem cells (ADSC) the umbilical cord also has stem cells. BioBurst Rejuv has considerable research showing that not only does their processing provide stem cells for injection, but they also have demonstrated high degrees of stem cell activation and proliferation. They have also shown that in the BioBurst processing technique they have isolated growth factors and cytokines that stimulate stem cell activation. Such injections can be useful for reduced scar formation and improved scar appearance.
Another useful enhanced wound healing agent is BioBurst Rejuv. This is an umbilical cord blood (UCB) derived cellular allograft which has been shown to initiate regeneration of soft tissue. When applied into surgical site it uses the body’s own natural healing process to signal molecules to initiate a regenerative response. Essentially signaling molecules recruit the body’s stem cells to the site of injury and cause them to proliferate. These stem cells promote a regenerative response with the formation of matrix proteins and blood vessels. While much attention has been given to adipose derived stem cells (ADSC) the umbilical cord also has stem cells. BioBurst Rejuv has considerable research showing that not only does their processing provide stem cells for injection, but they also have demonstrated high degrees of stem cell activation and proliferation. They have also shown that in the BioBurst processing technique they have isolated growth factors and cytokines that stimulate stem cell activation. Such injections can be useful for reduced scar formation and improved scar appearance.
The power to ‘heal thyself’ is no better illustrated in plastic surgery than in the potential of two popular and well-marketed natural body components, stem cells and platelets. Since these are located throughout the body in vast numbers and can be harvested and concentrated into injectable forms and put back into the same person, they are known as autologous healing or enhancement therapies. Both have become very popular in plastic surgery for use in a wide variety of reconstructive and aesthetic applications.
Stem Cells
While the use of embryonic stem cells in curing certain diseases is controversial, the use of adult stem cells for their potential cosmetic and anti-aging effects is no less debatable. Harvesting fat through liposuction as a source of stem cells, they are then ‘recycled’ and put back into the patient in the form of an injectable composition, with the assumption that tissues can be repaired, built back up or maintained. Numerous anecdotal claims are made about such injections creating youthfulness, adding permanent volume and improving the appearance of the skin. This has led to a number of touted procedures carrying such names as stem cell facelift, stem cell breast augmentation and stem cell-enriched fat grafting.
Most of the time such stem cell injections are nothing more than fat injections, which unavoidably contain stem cells. In other cases, the injections may be derived from fat grafts that have been processed through machines used to isolate fat stem cells by spinning the fat to separate the layers (although such machines have not been cleared by the FDA). While such ‘stem cell’ injections are unlikely to be harmful, they have not been proven to have anti-aging effects.
But are such touted stem cell procedures in plastic surgery believable? There is no doubt based on current research findings and direction that stem cells will eventually have a significant impact on the ability to regenerate tissues and may even have very observable anti-aging effects. But there is very little data from human clinical studies that currently support any of the hype or marketing claims some doctors make. Injecting stem cells under the skin has not been proven to improve the appearance of the overlying skin; there just isn’t enough evidence yet that it is effective. The clinical results to date are anecdotal, and years of research are still needed to figure out what stem cells can and cannot do. When used today, they should be done with the understanding that they are a lot like chicken soup – it can’t hurt, and may even possibly help.

North Meridian Medical Building
Address:
12188-A North Meridian St.
Suite 310
Carmel, IN 46032
Contact Us:
Phone: (317) 706-4444
WhatsApp: (317) 941-8237