Migraine Surgery
Migraine Surgery
 Migraines are one of the most common forms of head and neck pain. It is estimated that they occur in about 15 percent of people, with women being far more affected than men. The types of migraines vary from one person to another, with different symptoms and countless triggers.
Migraines are one of the most common forms of head and neck pain. It is estimated that they occur in about 15 percent of people, with women being far more affected than men. The types of migraines vary from one person to another, with different symptoms and countless triggers.
Fortunately, migraines can be controlled with medications that either terminate the attacks or prevent them from starting. However, some patients have not found adequate control or prevention on any type of drug regimen. And some well-controlled patients do not like the side effects of some of the medications, even when they are effective.
PERIPHERAL NERVE COMPRESSION AS A CAUSE OF MIGRAINE HEADACHES
In some patients, migraines are caused by the irritation of certain nerve endings in the head and neck. This irritation is caused by the muscles through which these nerves pass. The muscles pinch the nerves, causing inflammation and compression that can lead to a full blown migraine attack. These nerve endings are located in well-identified areas of the head and neck and are divided into four specific zones known as the frontal, temporal, occipital, and nasal areas. These are known as peripheral migraine triggers.
HOW MIGRAINE SURGERY WORKS
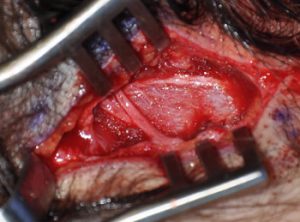 The principle of migraine surgery is to relieve the compression or squeezing of the nerves by the muscles. Releasing pressure on the nerves can prevent migraine attacks from starting, or at least weaken the trigger so that the migraines become less frequent and severe. These trigger points are first identified by Botox injections into the trigger point areas. If a patient has a positive response (migraine relief), then these trigger points can be surgically treated through small incisions hidden in the temporal and occipital hairlines. The squeezing part of the muscles can then be either partially or completely removed in order to alleviate the trigger point. In some instances, if the nerve is small enough and no harm is caused by its loss (temporal zone), the nerve’s endings are also removed. Either way, these surgical maneuvers prevent the migraine from recurring.
The principle of migraine surgery is to relieve the compression or squeezing of the nerves by the muscles. Releasing pressure on the nerves can prevent migraine attacks from starting, or at least weaken the trigger so that the migraines become less frequent and severe. These trigger points are first identified by Botox injections into the trigger point areas. If a patient has a positive response (migraine relief), then these trigger points can be surgically treated through small incisions hidden in the temporal and occipital hairlines. The squeezing part of the muscles can then be either partially or completely removed in order to alleviate the trigger point. In some instances, if the nerve is small enough and no harm is caused by its loss (temporal zone), the nerve’s endings are also removed. Either way, these surgical maneuvers prevent the migraine from recurring.
THE SUCCESS RATES OF MIGRAINE SURGERY
While migraine surgery can provide some spectacular cases of migraine relief, it does not always result in a permanent cure. Recent studies have shown it only achieves a complete cure in about one-third of patients. However, more than 90 percent of the time, patients do experience a reduction in the number, intensity and duration of migraine attacks. With the pressure off of the nerves, they are more resistant to migraine triggers.
BOTOX AS AN INDICATOR OF MIGRAINE SURGERY SUCCESS
 Like any pain reduction surgery, there is no guarantee of success and one would like to know what the likelihood of improvement would be with their unique migraine headache problem. A good way to test the potential success of peripheral trigeminal nerve decompression surgery is Botox injections. Since the culprit in peripheral nerve compression is largely the surrounding muscle, relaxing the muscle with Botox injections first is a good initial test or surgical ‘dry run’. Positive Botox responses almost always indicate a high degree of migraine symptom reduction with surgery.
Like any pain reduction surgery, there is no guarantee of success and one would like to know what the likelihood of improvement would be with their unique migraine headache problem. A good way to test the potential success of peripheral trigeminal nerve decompression surgery is Botox injections. Since the culprit in peripheral nerve compression is largely the surrounding muscle, relaxing the muscle with Botox injections first is a good initial test or surgical ‘dry run’. Positive Botox responses almost always indicate a high degree of migraine symptom reduction with surgery.
Before Migraine Surgery
Identifying the trigger zone is critical prior to migraine surgery. In most cases, this requires Botox injections to determine that the muscles are responsible for the trigger points. These include the following four zones.
Frontal Zone
 If most of your headaches start around the eyebrows or between the eyes, these are known as frontal or forehead migraines. In frontal migraines, the supraorbital nerve, which comes out of a hole in the brow bone, can be squeezed by the corrugator muscle (also known as the frown muscle). The peripheral trigger theory of migraines was discovered due to frequent cosmetic treatment of this area with Botox to preventing glabellar furrowing and frowning.
If most of your headaches start around the eyebrows or between the eyes, these are known as frontal or forehead migraines. In frontal migraines, the supraorbital nerve, which comes out of a hole in the brow bone, can be squeezed by the corrugator muscle (also known as the frown muscle). The peripheral trigger theory of migraines was discovered due to frequent cosmetic treatment of this area with Botox to preventing glabellar furrowing and frowning.
Temporal Zone
 If most of your headaches start in the temple area, or the side of the head, they are known as temporal migraines. There is a significant association in patients who also suffer from temporomandibular joint disorder (TMJ) pain and bruxism (grinding of teeth). Temporal migraines are caused by the zygomatico-temporal nerve being pinched by the temporalis muscle on its way to the skin.
If most of your headaches start in the temple area, or the side of the head, they are known as temporal migraines. There is a significant association in patients who also suffer from temporomandibular joint disorder (TMJ) pain and bruxism (grinding of teeth). Temporal migraines are caused by the zygomatico-temporal nerve being pinched by the temporalis muscle on its way to the skin.
Occipital Zone
 If most of your headaches start in the back of the head at the base of your skull, these are known as occipital migraines. Patients with occipital migraines will also frequently suffer from neck and upper back (trapezius) pain. In occipital migraines, the greater and/or lesser occipital nerves are pinched by an upper neck muscle known as the semispinalis capitis muscle as well as tight fascial attachments of the muscle to the base of the occipital skull.
If most of your headaches start in the back of the head at the base of your skull, these are known as occipital migraines. Patients with occipital migraines will also frequently suffer from neck and upper back (trapezius) pain. In occipital migraines, the greater and/or lesser occipital nerves are pinched by an upper neck muscle known as the semispinalis capitis muscle as well as tight fascial attachments of the muscle to the base of the occipital skull.
Nasal Zone
 If most of your headaches are located behind the eyes and around the nose, they are known as nasal migraines. They are caused by the nerves in the nose being pinched by a deviated nasal septum. These are often weather dependent and get worse when the nose is congested. Unlike all other zones, Botox cannot be used to identify this trigger point. An intranasal examination and CT scan are needed to determine if a severely deviated septum is the reason for the migraines.
If most of your headaches are located behind the eyes and around the nose, they are known as nasal migraines. They are caused by the nerves in the nose being pinched by a deviated nasal septum. These are often weather dependent and get worse when the nose is congested. Unlike all other zones, Botox cannot be used to identify this trigger point. An intranasal examination and CT scan are needed to determine if a severely deviated septum is the reason for the migraines.
Some migraine surgery patients will have more than one zone for the source of their migraine headaches. This is often present when migraines are unilateral, or located on one side of the head.
About Migraine Surgery – The Operation
Frontal migraine surgery is performed through small incisions hidden in the scalp to reach the corrugator muscles. (endoscopic approach) In some cases, the nerve may be approached from below and can be combined with cosmetic eyelid surgery or a cosmetic brow lift, if desired. Both sides are treated even if the migraines are only on one side to avoid an asymmetry of brow movement.
Temporal migraine surgery is performed through either an endoscopic browlift approach or an upper eyelid incision to reach the zygomatico-temporal nerve as it courses through the temporalis muscle at the side of the eye socket. In some cases, an incision is made in the temporal scalp to decompress the auriculotemporal nerve as well.
Occipital migraine surgery is performed through small incisions in the back of the scalp at the lower hairline. The semispinalis capitis muscle is removed from around the greater occipital nerve. Surgery may be done on just one side or both sides based on the patient’s symptoms and the results of the Botox test.
Nasal migraines are treated by a septoplasty procedure. The deviated portion of the septum is removed where it touches against the inferior turbinate bone inside the nose.
After Migraine Surgery
All incisions used for migraine surgery, either in the upper eyelid or in the hairline, are closed with dissolvable sutures. No dressings or wound care are needed. Migraine surgery patients can shower and wash their hair the very next day. There will be some mild discomfort at the scalp incision sites, but the swelling and bruising is very minimal. When upper eyelid incisions are used, one can expect some moderate upper eyelid swelling for a week after surgery. There are no physical restrictions or limitations after surgery. Some numbness will be present around the incision sites for a few months. Most patients experience an immediate improvement in their migraine headaches although the full benefit of the migraine surgery may take weeks to be fully realized.
Cost of Migraine Surgery
The cost of migraine surgery may be covered by your health insurance although this is uncommon. This can only be determined by a pre-determination letter written by Dr. Eppley. Often times, however, insurance denies these procedures as investigational or experimental even though their effectiveness is well established.

North Meridian Medical Building
Address:
12188-A North Meridian St.
Suite 310
Carmel, IN 46032
Contact Us:
Phone: (317) 706-4444
WhatsApp: (317) 941-8237
